|
Tips to make nail trimming a piece of cake!
How to work with your pet to make nail trims easy as cake! Relieving stress from your puppy or dog when it comes to nail trimming will help make them more confident and cooperative. Your pet is never too young to introduce them to nail trimming. Make sure it is a positive experience. Have plenty of your pets favorite treats.
0 Comments
.Topical minoxidil is a medication for hair loss, since 1996 it has been available as an over-the-counter product. According to a retrospective study in the Journal of the American Animal Hospital Association by Kathy C Tater, Sharon Gwaltney-Brant and Tina Wismer pet owners should be educated on the risk of dog and cat toxicosis from accidental minoxidil exposure.
Cat exposure was unintentional and usually while their owner was applying minoxidil for his/her own hair loss. The cat licked the owner's skin or pillowcase, or the pet was splashed during a medication spill Dog exposure commonly happened because of exploration behavior, meaning searching through trash. Clinical signs occurred in dogs and cats even with low exposure amounts, such as drops or licks. In patients that developed clinical signs, most developed moderate or major illness. Death occurred in 12.9% of cats that developed clinical signs after the pet owner's minoxidil use. Avoidance is the best plan. Other commonly used human medication can also cause toxicosis in our pets such as hormone replacement therapies, and topical 5-fluorouracil (5-FU) Signs & symptons of cat poisoning
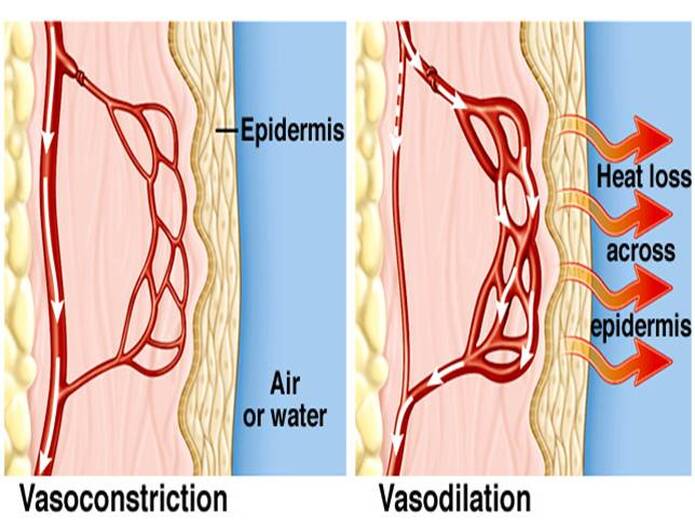
As heat waves spread across the state, and temperatures reach well into the 100's, it is important to keep yourself safe. But how often do we think about our pets in this weather? Our dogs and cats do not have the benefit of being able to take their fur off when it gets too hot like we can do with our clothes, so it's time to talk about how they keep cool! This post will cover how our pets stay cool (for dogs and cats), some symptoms of various heat related issues, as well as what you can do to help your pet. As the sun shines and temperatures rise, our pets figure out how to stay cool the best they can. Both dogs and cats will move to cooler spots where shade or grass is abundant, as well as physiologically changing their bodies to stay cooler. Dogs will typically pant to stay cool, while cats typically groom themselves more frequently.  Our pets can figure out where shade is, as that is preferable to the sun when it is hot outside. They also prefer grassy areas rather than concrete, so the ground doesn't burn their paw pads. If you are walking your pet, even in the evening when it might feel cooler, make sure to check the concrete by putting your hand on the concrete and keeping it there for 5 seconds. If it feels too hot, then it is too hot for your dog! Imagine walking on the hot concrete bare-footed for 20 minutes rather than 5 seconds if it feels too hot. It could get uncomfortable and potentially cause a burn on their paw pads, which can lead to worse problems if not treated. Never underestimate the power of waiting an hour when it comes to taking your dog on a walk to avoid the heat. The physiology involved in keeping cool is actually very interesting! In times of hot weather, the blood vessels will actually dilate to help direct the blood more towards the skin. By directing the blood more towards the outside surface, the blood gives off heat which travels through the skin and is emitted outside the body. Heat that gets emitted outside the body does not get circulated back into the system, so the pet cools down. This is why our pets (and us too!) appear red on their skin when it is very hot outside. It is a sign that the body is doing everything it can to get rid of heat, and that should be a sign to get your pet to a cooler area with water and shade available.  Although our pets sweat through their paw pads, it is not the primary way that they use water to help keep cool. The sweat on their paws is mostly used for traction on the floor. Dogs will pant when they are hot, which works because the water on their tongue evaporates, taking some of the heat with it. Some dogs are better at this than others, with brachycephalic (short nosed) breeds having a harder time panting and breathing in general. This would be your pugs, bulldogs, and boxers. Panting also helps get a larger amount of cooler air into the body system. Cats don't typically pant unless is is very hot, but they will groom themselves more in the summer. As they lick their fur to make it wet, the water evaporates, again taking some of the heat with it. If you see your cat panting, it is time to get them inside where it is cool and get them plenty of water, as that could indicate the potential for something worse to happen. The amount of variety with how our pets can stay cool is, well, pretty cool! Clinical signs of your pet in the heat can vary in severity and duration depending on what is happening, and they can be anywhere from a mild irritant to life threatening. That being said, prevention is every ounce more valuable than treatment, so do try to keep the heat in mind as you do your outdoor activities.  Heat Exhaustion (also known as heatstroke) is where your pet overheats after being in the sun or warm temperatures too long. Normal temperature ranges for cats and dogs vary from 100.5 to 102.5, where anything above 102.5 is considered higher than normal. Symptoms that are mild can progress to more severe issues quickly when heat is involved, so it is important to look out for mild symptoms and act on it quickly before it becomes a problem. Symptoms you may notice at first include:
If you recall, the blood vessels can dilate to help blood get to the surface of the body. The veins can also constrict to force blood to keep away from the skin to stay warm. When you dump really cold water on your pet, the veins constrict, keeping blood away from the skin, so they cannot cool down that way. The secondary problem with this is that it also causes the local blood pressure to rise, forcing the heart to pump harder to make up for the new resistance it is encountering. This can lead to cardiac arrest if a great enough area of dog is covered in cold water - full submersion would be worst case scenario here. To prevent this just use warmer water! Water that is cool but not cold will help mitigate the chances of shock and help keep your pet cooler without any risk. The process of evaporation works wonders over time, and the other measures you take will help your pet in the short term until it takes effect.  Speaking of water, dehydration is another problem that can happen with hot sunny days. Your pet could be dehydrated if:
 Something less common that could still happen is a sunburn on your pet. For dogs and cats this does not typically happen anywhere besides their nose, as they usually have enough fur to block out the sun. It is not a bad idea to use sunscreen safe for pets on their noses - this does not have hair protecting it, although a major problem with this is that the nose is awfully close to the tongue, and if they feel something on their nose they tend to lick it off. If your pet has short hair that is very thin, or no hair at all, like our sphinx cats, then sunscreen over the whole pet is definitely warranted. Again, make sure it is pet safe. If you don't have any on hand, you can use the sunscreen that is made for kids, as these typically have a decreased amount or no trace of harmful chemicals, such as oxybenzone. And of course, make sure you have a shady spot nearby.  One thing that summers and dry weather do is kick up weeds that have spines, needles, or hooks on them. While nature is effective in helping these plants get around, nothing is more frustrating to an owner (and us honestly) than a grass seed, foxtail, or many of the other names that basically mean "grass splinter that is embedded in pet". These typically get caught in the ears or between the toes of your pet, and cause irritation, swelling, infection, and constant itching. If you notice these signs at all, make an appointment with a veterinarian to have your pet looked at. These cases sometimes require sedation to remove the grass seed if it lodges itself in the body deep enough, so be prepared that this may be the case. The only way to avoid these is to stay away from tall grass and weeds, but this can be easier said than done. It is always helpful to know the signs and symptoms and act on it when appropriate. Hopefully this post was insightful on how to help your pets stay cool. The heat waves are not an environmental condition to take lightly, and so it becomes imperative that you are well prepared. When it feels too hot for you, it is likely too hot for your pet. Keeping shade and water nearby, and checking in with your pet to make sure that they are doing oaky is the best way to go about handling the heat. If at all possible, stay indoors at the hottest times of the day, usually between noon and 5:00 p.m. Preparedness saves you a lot of trouble later down the road, and it can't hurt to have an extra bottle of water on hand for your pet. Hopefully the heat waves abate soon, but in the meantime stay safe and use good judgement! Have a safe and wonderful summer!
 When you think about insurance, what are the first couple of words that come to mind? Do they involve positive, educated feelings about what insurance is and the benefits associated with it? Do they involve negative connotations of cost or dishonesty? Or do you scratch your head and wonder where to begin as far as talking about insurance? It can be a daunting topic to discuss, because there are so many legal rules to be aware of, and that's before you even begin discussing a policy with an agent. It can also seem useless at times, especially if you have not had any accidents or need for insurance recently. Pet insurance is no exception, with as little as 1.7% of all pets being insured in the United States. In other countries, such as the U.K and Sweden, these numbers are often in the double digits. With so little usage in the U.S, it is understandable why pet insurance is not often talked about or even understood. This blog article will discuss what pet insurance is, the different options available for insurance, as well as how owners can become more educated about insurance for their pets. There are many companies out there that offer pet insurance, and it is good to know the basics before you begin discussing the benefits of having pet insurance and which companies to consider.  Insurance is where you pay a premium, often monthly, to a company in order to receive financial compensation or financial coverage in the case of an illness or accident. Pet insurance, by extension, is simply where you pay for coverage on your pet in case they get sick or hurt. Depending on the policy you sign up for, your premium may be low monthly payments, with the caveat that they will only cover 70% of costs. Alternatively, the company may pay for all expenses after a certain point you pay up to, called a deductible, as long as you make your monthly payments. Often these premiums are higher, but can be beneficial for covering larger unforeseen expenses. Balancing the best plan for your budget and pet comes down to your personal decision as a pet owner as well as what your budget will allow. Typically, it is best to set the deductible no lower or higher than the highest amount you are willing to pay out of pocket for your pet. By doing so, you can feel better about when insurance is called in, as you have previously already decided what your limit should be.  Pet insurance is worth it for the same reasons that health or auto insurance is worth it for humans. Though it costs money each month, it allows for coverage of unexpected costs, such as a broken limb or serious illness. We cannot plan when these injuries or illnesses will happen, but putting money into insurance gives comfort and peace of mind knowing that, should an emergency come up, expenses will be less at the forefront of your medical decisions for your pet. Pet insurance has been proven to reduce the occurrence of economic euthanasia, where a pet is euthanized because the owner is financially unable to take care of it anymore, regardless of its age. These are tragic events, and can be prevented if insurance was utilized to help cover medical costs, particularly later in life. By taking the financial burden off owners, most pets can live longer, healthier lives due to the better care they receive.  An argument can be made for putting money into a separate pet savings account, where you can pull out the money only for the pet. While on paper this idea is a good one, the downsides may discourage you from opting into a "DYI" insurance plan. One downside is that if you decide to go with this plan, you need time to accrue enough money to prepare for an emergency. If you decide to start putting in $100 a month into an account for your pet, but your pet gets into an accident that costs $2,000 to fix a month later, you do not have the financial strength of that account to cover the costs. In doing the math, you would need another 19 months to save enough money for that expense, in which time the pet could get into another accident, costing even more money! Insurance is useful in preventing these instances by offering coverage as soon as you sign up, depending on the company. This means that as soon as you are approved, you will get the money needed for that accident, regardless of when it happens after you are approved. The best treatment for your pet at a fraction of the cost you would pay out of pocket is now within reach, because you bought insurance. A win-win for your pet and your wallet! Some owners may offer the argument that their pet does not go outside of their home and will not get sick or injured due to a lack of real threats from the outdoors. These owners should be aware that many diseases and injuries can happen whether the pet is indoors or outdoors, such as hypothyroidism, Addison's disease, or even accidents such as broken limbs or lacerated soft tissue. Illnesses can become lifetime diagnoses, where lifelong medication is required. Without insurance, the bills can add up quickly for pills and testing. With insurance, the cost is mitigated and you do not have to put off important testing for your pet to make sure the right treatments are being given. By getting insurance, you can help ensure that your pet receives the care it needs regardless of the financial cost, depending on your insurance plan. Many times in the hospital we see small dogs presenting for limping or lameness, where the only incident that may have occurred is the dog jumping off the couch or bed! It is impossible to create a home that is 100% safe for the dog or cat while keeping its mental health as a priority. This means that no matter your home situation, the chances of a hurt limb are still present. While it is important to keep your home as pet friendly as possible, the risk still remains no matter how small. Insurance will help mitigate the financial damage from those incidents, and allow you to focus on getting the best care for your pet, which allows for the best chances of healing properly and making a full recovery.  There are plenty of different pet insurance companies available in the United States, each with their own perks and company-specific plans available for pet owners. I believe that four stand out as a good variety of insurance that covers a wide variety of needs: Trupanion, ASPCA Pet insurance, PetsBest insurance, and HealthyPaws Insurance. These four can be compared, along with many others, at this website - https://petinsuranceinfo.com/pet-health-insurance/compare-providers . Each company has many different options and the only way to find out which is best for your pet is to decide for yourself what is affordable and reasonable coverage for your pet. Remember to take your pet's age, breed, and pre-existing conditions into account before making a decision - some of these companies will not cover these or charge extra. Ultimately, the decision should be yours to make, as long as you feel they will be able to supply the best insurance care for your pet. Treat your insurance search like your search for a good vet. Your pet's health should always come first! With a wide variety of plans including sickness and accident, accident-only, sickness-only, or a wellness plan, there is an insurance company that can fit your needs. Pet insurance should be obtained as early as possible. If your pet is older, it may have already developed conditions that are lifelong and require treatment, which may prevent certain insurance companies from writing a policy for your pet. By getting insurance when your pet is healthy and young, you can ensure that you have a policy prepared in the case that your pet gets injured or develops a severe illness. This also helps protect your puppies, as the most expensive year of owning a dog is typically the first one. This is because puppies have a tendency to eat things they shouldn't and injure or break limbs. With pet insurance, you can have peace of mind knowing that should your pet get injured unexpectedly, you have the means to help cover the expenses. Whether you have a dog, cat, or other pet, there is an insurance company that would be able to help you find a policy that best fits your needs. There are an astounding number of benefits that come with pet insurance, but it all boils down to taking care of your pet with the best methods available. With pet insurance, you can get access to treatment options and plans that may have not been possible otherwise. It is not very difficult to look up different companies using the links below, and they are willing to explain to you what the different policies mean. With a little bit of research, you might be surprised at the plans you can afford!
To Our Clients, We hope you are faring well. As each week goes by we know the measures we take to keep you and our staff safe have been cumbersome and tiring. Keeping our veterinary clinic open to care for our patients has been our top priority. To keep you and our staff safe and continue to maintain high-quality care (which is something none of us are willing to compromise on), we are limited to the amount of patients we can care for in one day. This means scheduling several weeks in advance for wellness exams. Often we are unable to accommodate same day visits. We are scheduling 2-4 weeks out for wellness visits and 3-6 weeks for surgical procedures. Due to social distancing, phones and online communication have been heavily relied upon for communication which has resulted in increased phone volume, wait times or not being able to get through to us at all. We apologize for these frustrations and hope you realize we are doing the best we can. As a clinic we have come-up with solutions to mitigate these challenges. Below is a list of alternatives to hopefully make your visit with us easier:
To assist everyone during this pandemic, we are asking the following of you:
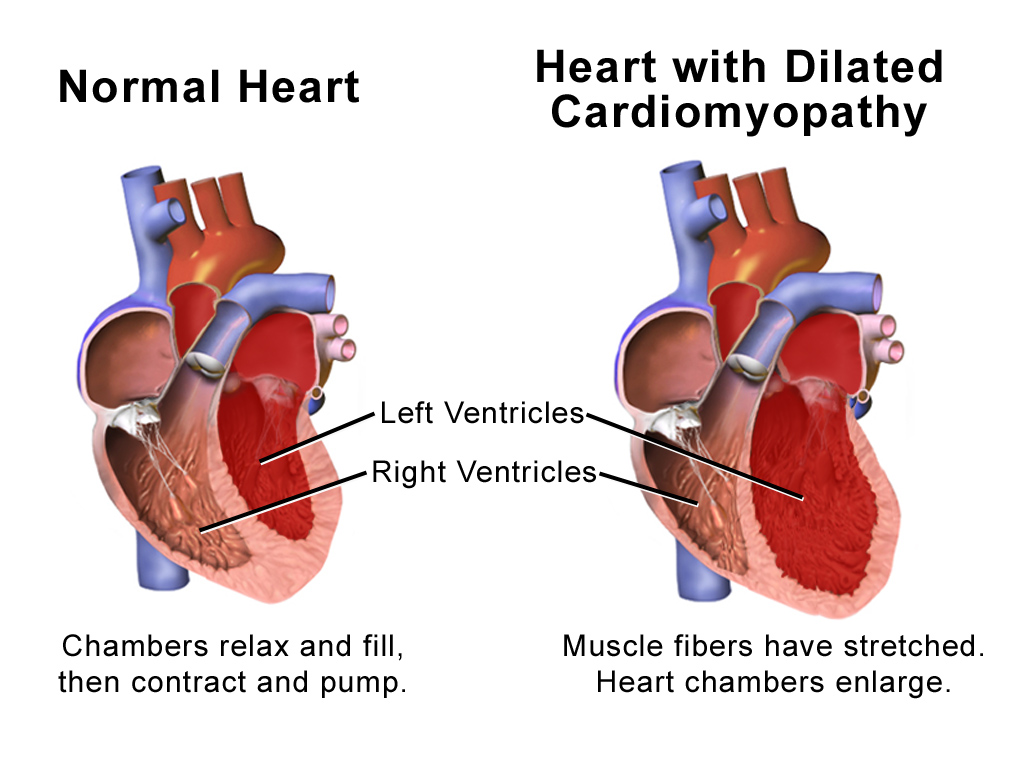
Thank you so much for your support and understanding. Please stay safe, keep your pets safe and know that we are always doing the best we can for you. North Ogden Animal Hospital “I won’t let pain turn my heart into something ugly. I will show you that surviving can be beautiful.” -Christy Ann Martine To Free or Not to Free: The dilemma with grain-free foodPet food, specifically dog and cat food, has been a hot topic of research for its pertinence and complexity. Many owners want to give their pets the best care they deserve and this can be easily done through pet food, which is easy to understand on a basic level and is easy to administer for the owners. However, some foods may be harmful to our pets and could cause damaging diseases later in our pets' lives. One such controversial food that has been a hot topic of research recently has been grain-free food. Grain-free food is food that does not contain any grain or grain-based products, whereas grain-based food does contain grain or grain-based products, such as wheat, barley, and oats. Grain-free foods are varied in appearance and usually a main ingredient is used in substitute for the grain in a grain-based food. Some examples are duck, carrots, potatoes, peas, sweet potatoes, or even exotic meats such as kangaroo! Sometimes exotic ingredients in foods are referred to as boutique or exotic diets because their main ingredients are less common. These ingredients are less studied and not much is known about them from a nutritional standpoint. Homemade or raw food can also be considered to be in the grain-free category. Oftentimes owners that make their pets' food do not consider putting in grains of any sort, and the raw diet consists solely of raw meats. These may also have the potential of causing debilitating diseases later on in life, and the connection lies in whether there are grains or grain-based products in the food or not. Grain-free foods may be potentially linked to an increase of heart disease known as Dilated Cardiomyopathy (DCM) which causes a weakening of the heart. This link was first suggested when veterinary cardiologists were noticing uncommon breeds and atypical cases of DCM presenting to the hospital more frequently. DCM begins when the heart begins to expand, or dilate, weakening the muscle wall as it does. This also causes the chamber within the heart to expand outwards and become larger, which causes the heart to have to work harder to pump the same amount of blood through the heart due to the larger chambers within the heart. This can lead to serious complications such as heart arrhythmia, congestive heart failure, or sudden death. The severity of this disease has prompted a closer look at how we can diagnose and treat this disease more efficiently. How could grain-free foods be linked to a complicated and problematic disease such as DCM? Some researchers are discussing potential hypotheses such as toxic components found in the grain-free foods that may not be present in the grain-based foods or nutrient deficiency that may be grain-free specific. The toxic component has not been found if one exists, however we have examples in the past of dog foods containing dangerous chemicals such as the melamine-cyanurate complex that was popular in pet foods and infant formula until the late 2000's. These examples lay the groundwork for potential investigations into the possibility that a cardiotoxic chemical found in grain-free foods may be harmful when consumed. Others surmise that a nutrient deficiency is the cause of DCM, and that there simply isn't the correct balance of nutrients in grain-free foods. In the past cats had a history of problems with DCM, until it was discovered that there was a deficiency of taurine in most cat foods. When taurine supplementation was added to the pets' diet, or the food itself had an increase in taurine, it was found to significantly reduce the amount of DCM cases in cats. Could this be the same case for grain-free foods because of a deficiency in taurine or some other essential nutrient? More research is needed, but we do know that age plays a role in the caseload of DCM - older pets are more prone to DCM because they are exposed to a diet for a longer period of time. Those that remain on grain-free diets for extended periods of time could be more vulnerable if the food was causing issues in the pets' health. We also know that different flavors of food change the bioavailability of nutrients in the food. Lamb and chicken flavored foods must be manufactured separate from each other if the food is to remain nutritionally sufficient, as lamb has more protein content than chicken. With this in mind, it may be that grain-free foods potentially are missing an essential nutrient or they have a mixture of nutrients that are reducing the nutrient bioavailability of the food. Either way, research into this field could bring promising leads into potential links between grain-free foods and DCM.  Regardless of the cause behind the potential link between grain-free foods and DCM, there are some barriers to getting the information out to our owners. Correct and scientifically sound numbers are difficult to come up with due to reporting bias. If there is a large population of golden retrievers, and only a few German shepherds and other breeds that are also reported, then the large amount of golden retriever cases can be partially explained by the large sample size. Research must be done diligently with respect to this bias in order to gather the correct information pertinent to the situation. Another barrier is the pet food marketing industry. Marketing has far outpaced research, and because of this, there are many foods that are marketed as safe and healthy with no scientific research or study to back up the claim. This is mostly seen in exotic ingredients, which do not have the same research and knowledge that other common ingredients have. Other foods may be marketing their nutritional value, while also lacking the capability to follow up on promises of healthy food due to facility structures and lack of proper monitoring. In both cases, greed outpaces research, and the recipient of this carelessness is our pets. It is important to ensure that the food you are feeding your pet is nutritionally sound and healthy. Speak to your veterinarian with any questions about any foods you are feeding your pet, as they can help point you in the right direction if you are feeling lost with all the pet foods and brands out there. There are lots of food brands, and it is important to do your research when you buy pet food.  It is clear that food choice and awareness about grain-free options are important to consider when feeding your pet. It should be noted that although grain-free food may be linked to an increase in DCM, it is not a guarantee that your pet will get DCM from grain-free food, only that it increases the likelihood of DCM diagnosis. In some cases, pets are allergic to grains, and in this situation it is up to the owner to determine what would be best for the pet. It is recommended that pet owners work with their veterinarian to find the correct solution for their pet. There are options to work around food allergies, such as finding grains your pet is tolerant to, or even getting allergy testing to discover what the allergy is comprised of then giving food that does not contain that specific grain. Regardless of the option you go with, avoiding grain-free food would be beneficial for your pets' health if at all possible. There may be some cases where grain-free food is a must for your pet, in which case it is important to continue to monitor your pet and ensure that veterinary visits are frequent enough to keep your pet safe. Ask your veterinarian for what they would recommend if this is the case. Giving an accurate diet history will also be helpful for getting the best advice from your veterinarian. With an accurate and complete diet history including flavors and specific brands, your veterinarian will be able to notice patterns and give you advice on what to feed your pet. Different flavors have different nutritional requirements and this necessitates some research into what would be best for your pet, which is furthered by a good diet history. It may also be beneficial to give your pet taurine supplements if you decide to give your pet grain-free food, although this should be discussed with your veterinarian beforehand. Though this isn't proven science yet, this was critical to helping cats avoid DCM as a common disease, and it may be the same case for dogs on a boutique, exotic, or grain-free diet.  It should be noted that DCM caused by food could potentially be reversed partially by switching diet to a grain-based diet. It is never too late to consider the care you are giving your pet and switch if needed. Early signs of heart disease include, but are not limited to, weakness, shortness of breath, coughing, fainting, or lethargy. If you notice any of these signs in your pet, and your pet is on a grain-free diet, it would be beneficial to schedule an appointment with your veterinarian to determine what should be done, if anything, to treat these symptoms before they worsen. As pet owners we are the advocate for our family, and we need to be monitoring and checking up on our pets to ensure that they are healthy, and be their voice if they are not. Discussion with your vet should be honest and open, with a goal of approaching the best care possible for your pet. Only by discussion and knowledgeable research can we figure out what's best for our pets. Ultimately the well-being of our pets is the primary reason for care and veterinary recommendations. Compliance with these recommendations will help support your pet's health and allow you to save money on future expenses to the hospital by taking care of your pet now before medical problems arise. Keeping grain-free foods out of your pets' diet should be a helpful first step to keeping your pet as healthy as it can be. By avoiding grain-free foods, listening to your vet for any recommendations, and keeping a keen eye out for any new research being done on grain-free foods and a potential DCM link, we can become better pet owners and take better care of our pets.
North Ogden Animal Hospital is open and available to help you and your pet.
In an ongoing effort to keep our community safe and offer a healthy environment for our clients, your pets, and our hospital staff, we are following the CDC, AVMA and our local government guidelines. If you are ill or have recently traveled to a hotspot, please call us for advice with your pet care needs. We have plans in place to help ensure your pet receives the care it needs. Pet visits are limited to one person. Upon arrival call from your car to let us know of your arrival. When your medical team is ready, we will notify you by phone with instructions for your visit. We are currently providing curb side delivery of pre-paid medication or food in our parking lot. Please respect the ‘social distancing’ recommendations and maintain a distance of 6 feet from others and refrain from shaking hands or exchanging hugs at our clinic. Facial coverings worn over nose and mouth are needed while in our building. No personal items can be kept with your pet while boarding or hospitalized, including blankets, beds, toys, collars, leashes, etc. Above all, we thank you for your understanding and please do not hesitate to call us with any questions. We care about you, we care about your pets, and our community. We will keep you posted as information and news is available from the AVMA, CDC, or the government.  Imagine you are preparing to go on a trip. You have your luggage packed in the car, your family is all sitting in the car waiting for you to get your last few items before you leave for your vacation to Hawaii! You go through your mental checklist of all the things you have prepared: Luggage, snacks, money, wallet, dog.... Suddenly you realize that you forgot your dog's vaccination information and health certificate! Unfortunately, health certificates are a long, involved process, and it is too late to obtain one for your trip to Hawaii. You will have to board your pet somewhere... Situations like this could happen to anyone. Getting all prepared for a trip only to realize that flights would require your pet to have certain health qualifications can be a surprise to some owners. This post will help guide you through what you need to do to prepare your pet for a trip out of state, or even out of the country. Travelling requirements for a pet can vary greatly depending on where you would like to travel. There are instances where travelling interstate can be more difficult to achieve with your pet than travelling internationally. As if travelling wasn't complicated enough, each airline may have different travel requirements if you are flying, and there could be a difference in laws that need to be followed if you were driving internationally or interstate. No matter where you travel, you should do your research on the location you are going to and keep your pet comfortable and well hydrated throughout the travelling process. It may be a good idea to take your pet on a drive around town first to see how travelling is handled. Knowing how your pet reacts in a travelling environment may help you discuss any medications that may be useful to your pet's comfort and safety with your veterinarian. Having comforting items may also be useful, if your pet likes snuggling with a stuffed animal or blanket. If you have a pet that likes to chew on and eat blankets, bones, or other items, it may be wise to not provide those for your pet until after the travelling is done. Ingestion of foreign bodies can be a serious medical situation, and travelling may put you in a place that does not have quality veterinary care available. Knowing your pet and how it will react while travelling will help you make some of these decisions on how to prepare your pet for travel.  With all the requirements that differ drastically between locations, you may be wondering how you can find out what requirements you need to meet before travelling with your pet. The United States Department of Agriculture has a good website that can cover your questions on legal requirements for health certificates and travelling with your pet, which can be found here- https://www.aphis.usda.gov/aphis/pet-travel. Regardless of where you travel, it is likely you will need a health certificate. Most airlines require one, and most states and all international travelling will require one. A health certificate is just certification from a veterinarian that the pet is healthy, along with any indications of disease that could be passed on to other animals. It is usually filled out for the most part by your veterinarian, although you may also need the state veterinarian to sign your paperwork as well. Because of the long bureaucratic process involved, it is recommended that you begin planning health certificate work with your veterinarian 8-12 months in advance. This ensures that all deadlines and requirements are understood, as well as the financial payments involved with various tests and procedures that need to be done. Some tests take a month or longer to be completed, and it is too important to not take precautions with how much time to allot yourself to getting the health certificate done. Travelling with your pet can be fun and exciting, and with a little work beforehand you can have a safe and relaxing vacation. With a health certificate, up to date vaccines, and a kennel set up, you and your pet are prepared for whatever the vacation brings. Have a safe spring break and travel well!
Vaccination is a topic often discussed in the animal hospital, but many owners may be getting them without knowing their importance or how they protect their pet from disease. Vaccinations are quite possibly one of the most inexpensive, effective methods of protecting your pet from disease and they can be easily renewed annually at your local animal hospital. An overview of vaccination and some important concepts surrounding the topic will be discussed in this post. 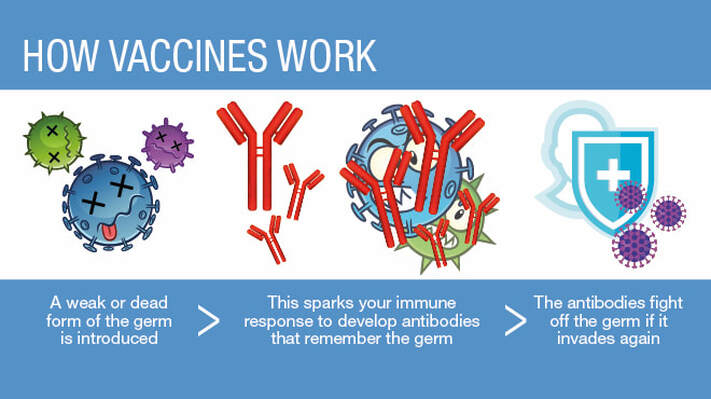 In order to understand the importance of vaccines, it can be helpful to understand how they work. Vaccines work by administering doses of antigens to your pet, normally through an injection, in order to 'train' your pet's immune system to fight off potential infection. These antigens basically consist of proteins that are found on the specific microbes that could cause infection to your pet, although vaccines typically make them weakened or reduce the amount of antigens first. When your pet is vaccinated, the antigens stimulate the body to produce antibodies, an important part of your pet's immune system. These antibodies perform many processes to prevent bacterial infection, including alerting immune cells to attack the bacterial cell, and forming a conglomerate of bacteria and antibodies to prevent the bacteria from moving and functioning correctly. Once produced, they can be remade in the pet's body whenever the infection comes back due to the fact that some cells that made the resistance to the antigens remain in the immune system. In short, vaccines work by introducing a small infection that the body is able to fight off. Once the body fights the infection, it can make more antibodies in case the infection comes back, thus 'training' your pet's immune system to fight specific infections.  Vaccinations are incredibly useful in preventing disease, but there are some important things to know about what may happen when your pet gets vaccinated. Your pet may have a local or systemic reaction to the vaccine, depending on your pet's specific immune response. Local reactions happen at the site of injection, and can typically consist of inflammation or vasculitis, where the immune system attacks the blood vessel by accident - the cause of this is unknown. Systemic reactions occur throughout the pet's body, and this can consist of symptoms such as anaphylaxis, hives, or GI distress (more common in cats). Your pet may be tired, sore, or have reduced appetite after getting a vaccine. This is normal and should go away after a couple of hours. It is important to note that any reaction to a vaccine is uncommon, and that the vast majority of the time your pet will be safe with the vaccinations your veterinarian recommends. On the rare occasion your pet does have a vaccine reaction, your veterinarian can prescribe treatments such as a steroid injection or antihistamine. These concerns should be discussed with your vet before your pet receives a vaccine if you have any concerns about vaccine reactions and your pet. Vaccinations are an important part of protecting your pet and helping it live the best life it can. By helping your pet's immune system recognize and build up defenses to threats before severe infection occurs, you are helping your pet protect itself. An important part of our job at North Ogden Animal Hospital is to ensure that your pets are taken care of, and vaccination is a treatment we advocate for to provide the best possible healthcare for your pet.
 Diabetes is a disease that is familiar to us as humans, but how much do we think about diabetic dogs? What about diabetic cats? This disease has been increasing in prevalence for both dogs and cats, although dogs are more prone to getting diabetes than cats. This blog post will discuss the nature of diabetes, how it affects dogs and cats, and treatment options for a diagnosed pet. To understand how diabetes is diagnosed, it is important to understand a little bit about the system involved with the disease. Diabetes mellitus is a disease where the glucose levels in the blood are elevated to dangerous levels. Glucose is the main energy molecule used by cells in the body, and it is taken up by cells as it passes through the bloodstream. In order to be taken up by the cells, glucose needs another molecule, insulin, to tell the cells to take up the glucose. In this way, glucose can be managed by the body as to where and when it gets taken up. There are two types of diabetes: Type I and Type II. Type I diabetes is where the pancreas, which produces insulin, is damaged or is malfunctioning and does not produce enough insulin for the body. This type of diabetes is most common in dogs. Type II is where the body does not respond appropriately to insulin. This is the most common type of diabetes in cats, although it is somewhat rare for a cat to get diabetes (less than 1% of cats are diagnosed with it). Both of these types of diabetes provide problematic situations for your pet; The cells do not absorb the glucose they need to fuel cellular processes, and the bloodstream cannot get rid of the glucose present. Glucose can then rise to toxic levels in the blood, which can lead to kidney, eye, heart, and nerve problems. 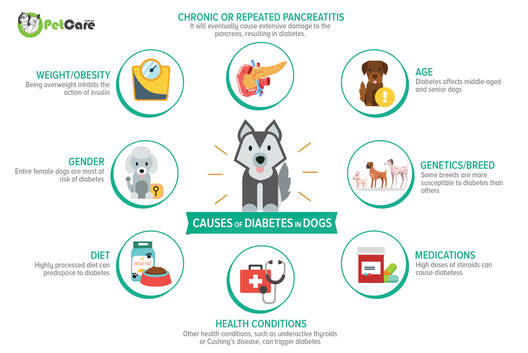 When a pet has diabetes, there are some clinical signs you can look for that may be a concern to bring up with your veterinarian. Some of the major signs are: -Excessive thirst -Increased urination -Unexplained weight loss -Increased appetite Lethargy and disinterest in activities may also be advanced symptoms of diabetes. With these clinical signs, they all tie into the body trying to get rid of the excess glucose in the blood, or showing adverse effects from not being able to use glucose that is present in the blood. The thirst is due to your pet urinating more, and the weight loss and increased appetite is from the cells not being able to grab the nutrients they need. Urinating more allows the body to dispel waste from the body, including excess glucose. The increased appetite can be misleading, as you may think your pet is starving and will want to feed him/her more food. In reality, this will only increase glucose levels in the blood, which can be dangerous, without providing much as far as nutrition goes because of the reduced amount of glucose being taken up by the cells.  There is no cure for diabetes, although there are many ways to improve your pets quality of life when it has been diagnosed with diabetes. Insulin injections are the most typical way of managing diabetes, and there are a wide variety of brands and insulin, each with their own pros and cons. Insulin injections are useful and common for managing your pets diabetes, and you can discuss with your veterinarian how to best manage your pet's diabetes. You can also check the blood glucose levels of your pet with a glucometer, a machine that checks glucose levels. It can be intimidating at first, but with a little practice and guidance from your veterinarian, it is an easy way to monitor how your pet is doing, giving you information to make a plan with your veterinarian to create a dose and plan catered specifically to your pet. Dietary management is important in maintaining weight for your pet. It is important to keep in mind that although your pet may have a larger appetite, the cells are not getting the glucose they need to function efficiently, and that will cause weight loss. A low carbohydrate diet may be prescribed by your veterinarian, which has been shown to help manage glucose blood levels better. Always follow your veterinarian's guidance on how diet is to be implemented in your pet's health plan. Diabetes is a disease that can be confusing for pet owners, and it is important to educate yourself as much as you can when your pet is diagnosed with diabetes. It may seem impossible to work with, but many pet owners are successful in giving their pets the best quality of life they deserve. Diabetes, although incurable, can be well managed with insulin, dietary management, and love from owners like you. With a little love and effort, your pets can live wonderful, fulfilling lives. Helpful Links: https://www.vet.cornell.edu/departments-centers-and-institutes/cornell-feline-health-center/health-information/feline-health-topics/feline-diabetes https://www.akc.org/expert-advice/health/diabetes-in-dogs/ |
Author:NOAH Staff Archives
April 2022
|